As of March 17, 4,226 cases of COVID-19, or the coronavirus, have been reported in the U.S. More than 75 people have died.
Dr. Stephanie Taylor, a graduate of Harvard Medical School, is the CEO of Taylor Healthcare Commissioning Inc. After working as a physician for many decades, Dr. Taylor obtained a master’s in architecture as well as an infection control certification. Her lifelong commitment to patient care includes focusing on improving the health care physical environment and clinical work processes to help patients heal quickly and save hospitals valuable dollars.
Recently, Dr. Taylor joined Herb Woerpel, editor-in-chief of Engineered Systems, for an episode of the Percussive Maintenance podcast. Here is a transcript of that conversation.
For access to more podcast episodes, click here.
Engineered Systems: Dr. Taylor, welcome to the podcast. Now I'm sure many who are listening are familiar with you through your IAQ column. But for those who are not, could you please take a moment to introduce yourself?
Dr. Taylor: Please, feel free to call me Stephanie. I’m a physician of many decades actually, and, while practicing a pediatric oncology, I became very concerned about the role of the building in my patient outcomes. So, I expanded my line of work to include architecture and engineering. And now, I'm very passionate about how important and powerful the indoor environment is on human health. I now have my own company that focuses on consulting and research. I live in Stowe, Vermont, and do my clinical work in Boston. Also, I’m very honored to write for Engineered Systems.
Engineered Systems: We’re honored to have you on our staff. Over the last several months, the world has changed significantly, all because of the novel virus COVID-19, better known as the coronavirus. So, what exactly is the coronavirus?
Dr. Taylor: The coronavirus is a whole family of viruses. It got its name because there are these little spiky projections on the outside of their viral envelope. I guess somebody thought it looked like a crown, so it's called a coronavirus, but coronaviruses are actually very common families of viruses. Approximately 30% of the common cold is caused by a form of coronavirus. However, this type of virus is an RNA virus. RNA is the type of genetic coding that is read when this virus replicates into baby viruses or many other offspring. RNA viruses mutate very easily and quickly because in that process of replication, the normal sort of proofreading mechanisms are not present. So, almost all of the pandemics we’ve experienced as human beings have come from RNA viruses — the influenza, Spanish influenza, Ebola, SARS, MERS, and now this one. We need to learn to deal with both the infections from RNA viruses as well as the environmental factors that promote these mutations that result in new diseases. But, to answer the question directly, coronaviruses are common. Their normal reservoirs are animals, like camels, cows, and sheep; however, as we have experienced with the cold, SARS, MERS, and now with this one, these infections are easily transmitted from human to human.
Engineered Systems: Do we know exactly where COVID-19 first came from?
Dr. Taylor: We definitely have some theories that it came from a meat market in in China. Looking at the genetic code of the viruses and the people it has infected, we're finding that they're not exactly identical to what we might expect, which has put that theory a little bit under question. So, we don't really know where this mutation occurred, or where this exact strain came from, but it does seem like it came from an animal reservoir in China.
Engineered Systems: There's a lot of misinformation floating around, and we've heard a lot of rumors. One in particular focuses on someone eating a bat. Can we put that rumor to rest?
Dr. Taylor: I think we can put that rumor to rest. As human beings, we want to assign blame to someone or something. I believe we need to just move on from that attitude. Where it came from doesn’t even matter. This is a brilliantly mutating coronavirus that has replicated in a unique way.
Engineered Systems: So when did you first hear of this latest strain of COVID-19, and what was your first thought or observation of it?
Dr. Taylor: I first heard about it in December. I think we were calling it the Wuhan virus at that time. My first reaction was, well, I'm not surprised. You know, again, RNA viruses mutate very rapidly. A new strain can take off and replicate very easily. Human beings don't have immunological memory against these strains, and we serve as a whole new set of hosts for these viruses to grow in. So, my first reaction was, I’m not surprised.
Engineered Systems: How has your opinion of the virus changed over time? Did you ever expect or think that it could reach pandemic status?
Dr. Taylor: I have to say I downplayed it more in the beginning than I am now. This is a very serious pandemic. I think the other factors that are going on right now, such as human fear, are playing a role. I think there are characteristics of this virus that undeniably make it frightening. I think this is an incredibly serious infectious outbreak, and we’re reacting as human beings to something we cannot easily control. So, I am taking it very seriously. At first I sort of thought, well, I'm immune, because I’m healthy, though I admit I’m not as cavalier as I once was.
Engineered Systems: Stephanie, how is this outbreak different from say some of the others we've seen in the recent past, like H1N1, Ebola, or even Polio?
Dr. Taylor: Great question, Herb. So, this virus is different in a couple of key ways. One of the biggest things is that people are very infectious for days before they're ever symptomatic. So, you may be spreading this virus for days before you even know you’re sick, which makes it hard to contain. Another thing about it is that when people transmit the virus through a cough or droplets, the concentration of infectious viruses is very high. One person can infect a lot of people. With most of the other illnesses we've encountered, there's a more immediate correlation between your symptoms and if you’re infected. So, with those illnesses, it's easier to say, OK, I don't feel great, I’m going to isolate myself.
Another difference is that this virus attaches really deeply to the receptors in your lungs. So, while the common cold more likely attaches to your sinuses and throat, this attaches deep in your lungs, which causes you to get sicker.
Engineered Systems: We're recording this on March 17. Happy St. Patrick's Day! And, at this point, several states have closed bars, restaurants, gyms, and theaters to dine-in customers and restricted meetings larger than 10. In your opinion, is this the right thing to do?
Dr. Taylor: Yes, this is probably the right thing to do, given that we don't know the extent of this pandemic. While we may never be able to stop the transmission, this will probably slow it down or flatten the curve, which we’ve grown all too familiar with. Any vaccine is still going to be 10-12 months away, but if we can further dilute the rate of spread, our health care facilities can ramp-up their intensive care unit beds or respiratory support. So, even though we don't really know the full dynamics of this, I believe this social distancing is a good thing to do.
Engineered Systems: You mentioned the vaccine is may be 10-12 months away. So, based on that information and the protocols that have been put in place, what type of timeline would you suggest we're looking at before this starts to dissipate? Two months? Six months? Longer?
Dr. Taylor: Using statistically based data, I think that it's hard to tell. I think there is going to be different phases of it. There may be an acute phase. Because we don't have an immune response that effectively fights this virus, there may be a phase where more people get really sick or die. Overall, this virus is going to live within our human population for a while. Hopefully, sooner than later, we'll have either a vaccine or develop more of our own defense mechanisms to fight against it.
I think the immediate, really frightening phase will probably wane over the next two months, which is just a guess. I do think that the summertime weather and a warming climate is going to benefit us. I think how we manage our indoor environment to decrease the extent to which we get sick will be a big part of what we can do as well. And if you live in New England, where I do, the weather is going to actually help control this. I don't think the weather is going to be the only answer, but I think it will help.
Engineered Systems: As consulting and specifying engineers and/or facility managers, what steps should we take personally and or professionally to combat this outbreak?
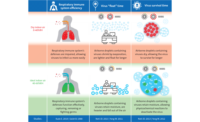
Dr. Taylor: That's a great question, and, luckily, we do have some strategies that can be used. It’s very clear that it's transmitted through the environment. And this is both alarming and good news. We've known for a long time that viruses can be spread through droplets. If somebody sneezes and one of those wet droplets lands on you, or a few feet away from you, and then you rub your nose or the virus or bacteria get into your body, you have a high chance of getting sick. But the transmission pathway that we haven't really wanted to think about is when an infected person sneezes, coughs, or simply breathes droplets into the air. If the air is dry, those droplets shrink and desiccate to reach a moisture equilibrium within the air around you. And we now know that the viruses in those very tiny desiccated particles can go up in the air, they can travel into an HVAC system, and re-infect people who are quite far away and have had no immediate contact. That's one of the things that makes this virus alarming. We can no longer deny airborne transmission of infectious aerosols. And even the CDC has waffled on this. They said the virus can be spread through airborne droplets, but that you don't have to worry about airborne transmission.
The concept of an airborne transmission of infectious droplets is scary, but we can help control it by — and anyone who reads my articles has probably gotten tired of hearing this — keeping the relative humidity in our breathing zone or in our buildings between 40%-60%. This has turned out to be the magic zone. I think Mother Nature gave us that opportunity so we could survive. If you're outdoors, even say in the winter, your relative humidity is typically in a fairly safe zone. It’s cold out and the low moisture content puts the relative humidity at 50%-60%. When we bring that cold air in the building, we warm it up to comfort temperatures, and all of a sudden relative humidity falls to 20%. And this is where we're getting into trouble. Data and research shows us that if people in offices, hospitals, and schools manage their indoor relative humidity at 40%-60%, humans’ mechanisms for physiological defense are improved.
There is some brilliant research from Yale that came out last May that really helps us understand how appropriate water vapor in our breathing zone bolsters our immune system. So, that's one mechanism. If you can humidify your indoor environment to this moderate zone, you actually bring out the infectious particles. They are brought down from the air. Research from 2010 as well as up to up to a week ago from the NIH [National Institute of Health], Princeton, and Harvard shows that viruses in the air and on surfaces are inactivated when the relative humidity is maintained in that zone.
So, while I understand some of the reasons why we’re kind of scared of humidity, or we don't like it, because we take it to high levels in our mind. The reality is, as human beings, we don't do well in dry air, and these quickly mutating viruses and bacteria do. In dry air, they're like, great, we can mutate, we can fly around, and we can find new hosts. So, one thing we can do is really think about the air. We can humidify from 40%-60%. There are other strategies, like UV-C light, which de-activates many organisms. Filtration can be very beneficial. Hydrogen peroxide misting is another one, and I’m sure I’m missing some. The one I like best is humidifying the indoor environment, because not only does it help support the air we breathe, it also bolsters our own immune systems, which is critical, especially now.
Engineered Systems: Now, I know we don't want to monetize this virus or disease at all, but as an HVAC designer or contractor, these solutions are certainly something I may want to pay attention to.
Dr. Taylor: Correct, I don't think anyone wants to benefit, and nobody wants this out there for our own personal benefit or gain, but it’s out there. We need to manage it appropriately. And, so, in a way, this is a very exciting time to be a mechanical engineer. Anyone in the building industry is now in the position to really be able to improve public health. You know, as physicians, we're kind of helpless. We can put people in respirators if we need to, give antiviral medications, and work on a vaccine, but none of that is going to be as effective as managing the indoor environment is right now. So, in a perverse way, it’s kind of an exciting time to be in the building industry — as difficult as that is to say.
Engineered Systems: So, obviously, washing our hands, proper hygiene, and proper Rh are all key as we continue to battle this, but do you have any other tips for those who may be listening to this podcast from their quarantined homes?
Dr. Taylor: Use common sense and try not to panic. If you're in the panic mode, your body is actually producing more cortisol, which is an immunosuppressant. We don't want to be immunosuppressed right now. So, try to not absolutely freak out. All of us are going to be anxious, and when you’re anxious to talk to people, call someone. Go out and get exercise, which is great. The improvements that come along with exercise are really good. Eat well and sleep well. Reconnect with your family. Wash your hands and humidify your home.
Engineered Systems: Anything else you'd like to add while we have you on the line?
Dr. Taylor: I really appreciate the opportunity to talk with you and with anyone who's listening. Please feel free to reach out to me with any questions. There are lots and lots of papers and research papers I could send to help answer any questions.
Engineered Systems: What’s the best way to connect with you?
Dr. Taylor: I use LinkedIn a lot. Also, my email address is MD@Taylorcx.com.
Engineered Systems: Fantastic. Dr. Taylor, thank you so much for your time. We appreciate you helping us try and decipher this coronavirus, and thank you for all you do for us at Engineered Systems.
Dr. Taylor: Well, thank you very much. Take care.
View more of Engineered Systems' coronavirus coverage by clicking here.