Good IAQ in these spaces is dependent on maintaining the quality of a number of variables. Most building occupants are familiar with temperature, humidity, and drafts. These three components combine to create the immediate feeling of comfort or discomfort in the building occupant. The building's heating, ventilating, and air conditioning (hvac) system is responsible for maintaining those variables in comfortable ranges for the occupants.
Odors also cause an immediate reaction to a building environment. Although they may be harmless, odors can be a significant distraction in the workplace. Odors may also be a sign of other problems in the workplace environment. They may indicate the presence of microorganisms such as mold and fungi, volatile organic compounds (VOCs) such as fuel or solvents, or irritating cleaning materials.
Other dangerous compounds such as carbon monoxide, ozone, radon, and many bacterial microorganisms have no smell or have an olfactory threshold below the danger point. Laboratory analysis is required to confirm the presence of these materials in the school or workplace.
Enter the IAQ Sleuths
In response to the increasing concern over the indoor environment and the identification of a myriad of factors combining to form Sick Building Syndrome (SBS), national IAQ testing services have continually increased their arsenal of approaches. Many of these procedures rely on relatively inexpensive testing devices that take samples of evidence to be analyzed later in specialized laboratories. This allows analysis to be conducted with sophisticated equipment that, although expensive to buy and difficult to maintain, provides the best possible accuracy.Other tests provide fast on-site analysis of possible problem materials, but they are inevitably less accurate than samples analyzed in a laboratory setting. Which type of test is best? That depends on the situation, and only the building operator can say for sure.
Identifying Microorganisms
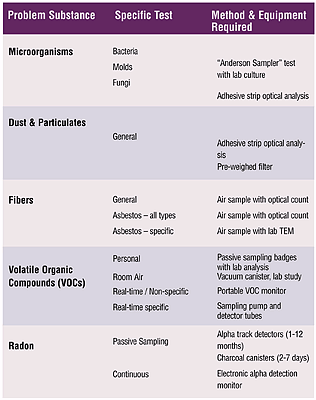
Microorganisms consist of bacteria, molds, and fungi. Their presence can cause irritation or allergic reactions that affect the eyes, nose, and throat. Although these symptoms may be confused with the common cold at first, lingering discomfort may point to an environmental cause. As a person becomes more sensitized, the symptoms get worse.The traditional testing method for microorganisms consists of the controlled exposure of a petri dish (or plate) containing a nutritional substance such as agar. Plates are exposed by loading them into a specialized air pump (the Anderson sampler), which draws air past the plates and impinges all airborne particles onto the plate. The plate is then sealed in an airtight, sterile canister for shipment to a laboratory.
Sampling plates are almost never exposed singly in the course of identifying a possible microorganism source in a building. If complaints point to a single classroom or office, that is where the samples are taken. But even a small classroom or office will require samples at two or three locations in the space.
The hvac system should be checked at the same time by taking a sample from the supply air duct where the air comes into the room. If there is an access hatch in the main supply duct entering the room (before the duct splits to several air supply diffusers or grilles) this is the best place to take the sample. This area should provide a consistent air velocity and laminar airflow into the sampling pump. If the supply duct is not accessible, the test should be taken at the supply air grille having the highest air volume.
A test should also be taken outdoors in the vicinity of the hvac outdoor air intake. This measure of the ambient microbial level is an important factor in evaluating whether the problem is inside or outside the building.
Finally, a control test should be taken somewhere else in the building where there does not appear to be an IAQ problem. An un-exposed plate is included with the exposed plates for each location as a control for the quality of the plates themselves. The plates are shipped to the lab with a packaged coolant to keep them below 40ûF.
At the lab, the disks are cultured in a controlled, sterile environment of 70ûF to 100ûF for three to six days and then examined under a microscope. The laboratory must be accredited by the American Industrial Hygiene Association (AIHA), which ensures that its equipment, personnel, and procedures comply with strict quality control standards. Without this or equal accreditation, the value of the testing is in doubt. (Note that the testing service provider also must be AIHA accredited.)
After culturing, the biologist looks for the growth of colonies of microbials spawned by the original particles from the tested space. The report then lists these results in terms of the number of colony forming units (CFUs) per sample divided by the total airflow in cubic meters (m3) drawn past that sample. Typical figures would be 100 to 10,000 CFUs/ m3.
These tests are time consuming. It takes about 10 minutes to expose a single plate. Each plate requires the sterilization of the sampling pump and a new set of sterile surgical gloves. Each location usually requires the exposure of several plates for control purposes. This adds up to 50 to 100 sample plates for a typical facility.
Because of the number of plates, the labor in taking the samples, and the culturing of the plates, this type of testing is relatively expensive with a 50- to 100-plate test running $5,000 to $10,000. Variation in cost is due to travel and preparation time necessary to gain access to the hvac system, outside air intakes, or closed building spaces.

Dust and Particulates: Weigh the Alternatives
The most common method of testing for particulate contamination is the use of pre-weighed sample cartridges. In this method, an air sample is drawn through a pre-weighed filter at a known flow rate for a measured period of time. The cartridge is weighed on a precision laboratory scale after the particulate has been deposited on the filter surface. The difference in weight before and after indicates the quantity of particulate in the air.The flow rate through the sampling pump is multiplied by the time the pump is operated to determine the volume of air sampled per m3. The final measurement of contamination is expressed in milligrams (mg) of material per m3. This is an integrated sample that only indicates an average particulate loading. It does not indicate anything about variations in particulate concentration with time. Nor does it indicate particle size.
Particle size is an important factor in IAQ studies. Particles of a size smaller than 10 microns are respirable and are a health threat. They are small enough to lodge in the lungs and resist removal by the body's natural mechanisms.
The Occupational Safety and Health Administration (OSHA) has established a maximum permissible exposure limit of 15 mg/m3 of nuisance dust based on an average eight-hour exposure. The American Conference of Government Industrial Hygienists (ACGIH) has established a maximum allowable level of respirable particulate of 10 mg/m3. The American Society of Heating, Refrigeration and Air-Conditioning Engineers (ASHRAE) recommends a maximum level of 0.15 mg/m3 for continuous exposure to respirable particles of 10 microns or smaller.
If particulate has been identified as a problem based on weight alone, further tests should be done to confirm what fraction of the particles is respirable. If the concentration is a great deal above 2 to 3 mg/m3, further tests should be done using cyclones or impingement plates to identify the size of the particles. If the particles are respirable, the cause should be corrected.
Asbestos and Other Fibers
Testing for asbestos has become a tried and true process during the past two decades. The procedure is to draw air through a sample filter and inspect with a microscope for the presence of fibers. This test usually takes longer to accomplish than air samples for microorganisms, but the setup and operation of the air sampling pumps is much simpler because no sterilization is required. The test usually takes about two hours, and several pumps should be placed throughout an area to get a good cross section of samples.The test filters are then examined under the microscope for the presence of asbestos fibers and the result reported in fibers per cubic centimeter (fibers/cc). This result will likely include all types of asbestos, some of which are not considered harmful. Nonetheless, the prudent owner will make every attempt to bring the total within the allowable limit of approximately .01 fibers/cc, regardless of the type of asbestos present. Asbestos in a school or workplace is too dangerous to permit a discussion as to the type of asbestos present. Also, the source of asbestos is usually relatively easy to identify and mitigate.
If large quantities of asbestos are present and disposal or other concerns call for an exact determination of the type of asbestos, samples will have to be sent to a lab for analysis by transmission electron microscopy (TEM). In most workplaces this should not be required and a thorough testing for asbestos should be possible for under $1,000.
Testing for fibers other than asbestos is done in a similar manner. A sample is taken and examined under the microscope to determine the fiber material. Then the percent by weight of the subject fiber as a portion of the overall sample is determined. The overall sample is then weighed and the weight of the subject fiber calculated. Examples of fibers of concern are filter media in hvac systems, insulation, and fireproofing. These are usually either fiber glass or a similar synthetic vitreous fiber. The OSHA allowable limit for these fibers in the workplace is 15 mg/m3 and the ACGIH allowable limit is 10 mg/m3.
Optical Sampling for Cost Savings
The use of an optical sampling cassette in combination with microscopic examination has increased in recent years. This is due to the continuing improvement of high-quality, optically transparent adhesive media that will trap airborne microorganisms, particles, and fibers.In this test, an air sample is drawn through a sterilized sampling pump and impinges on an adhesive surface. The adhesive surface sample (or cassette) is shipped to a laboratory where it is examined under the microscope. Technicians visually identify microorganisms, particles, and fiber on the sample and report back in terms of concentrations of microorganisms or fibers per m3 of air sampled.
Although this test covers a broad range of irritants associated with SBS, it is not as accurate as the other tests described above. This type of test has two main advantages: It provides a satisfactory level of accuracy at a modest cost; and it provides a broad indication of all suspended solids in the air and, as such, provides a good starting point for further testing.
If the optical test indicates very low levels, the investigator might be well advised to turn his or her efforts towards other causes such as VOCs. If the levels indicate a possible problem, further testing with cultured samples will have to be pursued.

The Badge Tells the Story
VOCs are organic chemical compounds in the vapor phase. They are usually the products of evaporation of fuels, solvents, cleaning chemicals, and vehicles for paints and finishes. VOCs are associated with any kind of vehicle or aircraft fueling station and are present in car, truck, and aircraft exhaust in the form of unburned fuel. They are present in most cleaning materials (although many such compounds have been banned in recent years). This includes floor and carpet cleaners, restroom tile cleaners, and desk, glass, and furniture cleaners. Finally, VOCs are present in most paints, stains, varnishes, shellacs, waxes, plastics, and other furniture room finishes. VOCs are present in the toner of most copying machines and ink of most computer printers.There are several methods of testing for VOCs. The first is to use passive samplers ("badges") placed in the suspected area for a day or so and shipped to a lab for analysis. These samplers may be worn by persons experiencing symptoms of VOC exposure, or they may be worn by all workers as a safety measure. They may also be mounted on walls, equipment, fixtures, or air supplies where VOCs are suspected. Passive samplers typically consist of an absorbent material such as activated charcoal sandwiched inside a semipermeable membrane. The VOCs pass through the membrane and are absorbed into the media.
At the lab, the absorbent media is emptied from the badge and analyzed by gas chromatography. The gas chromatograph produces a spectral graph of 50 to 100 chemical agents that may be present in the sample. A technician then studies the graph and reports materials that are present in significant amounts.
Passive badges are a good first step if VOCs are a suspected problem. They are easy to purchase and use. Typically, the cost of analysis is included in the purchase price of the badge.
The absorbent badge is a time-integrated sample. The badge will not record any variation of concentration with time. Rather, its sample will represent a sum total or integration of everything it has absorbed. This makes the badge useful as a first step in identifying the problem, but other more precise methods will be required to find the actual source of the problem.
The second method of testing for VOCs is to purchase a prepared canister from a laboratory, take a sample in the space, and return the canister to the lab for analysis. Taking the sample is easy because all of the air has been exhausted from the canister before it is sent out. All the occupant has to do is open the canister and let the room air fill it.
The canister method is an example of a "grab sample," a sample taken over a short amount of time that is representative of the air in a space at that time. This is useful if reported problems are related to a machine's cycle, a truck unloading, a tank venting, or some other transient activity. On the other hand, if the complaints are related to a long-term, low-level exposure, the grab sample is unlikely to provide the resolution necessary to identify the problem. The resolution of the canister is limited because it only holds a fixed amount of air, whereas the absorbent badges have an unlimited resolution in that they can be worn for as long as required to build up a detectable level of the target substance.
The third method combines the best qualities of both the passive badges and the grab sample canister. This is continuous or "real time" monitoring. Real time monitoring involves taking portable analyzers to the site and recording continuous measurements of levels of specific contaminants over time. This service is available but is expensive because it requires sophisticated equipment and trained technicians. Nonetheless, it might be the only way to correlate an odor or a transient contamination with a cause. Having a graph of concentration as a function of time is an invaluable tool in determining the source of the subject material.
The method that gives the fastest indication of VOCs is the use of disposable gas detection tubes. These can be purchased as required and are calibrated to show an approximate concentration of the VOC in the area at the time of the test. A detection tube is a grab sample device that is good for only one test. As such, they are too expensive to use for anything approaching continuous testing. A hand-operated pump is used to force the air sample past the chemical-filled tubes. The air sample pump costs about $500 and the most common indicator tubes cost about $10 to $20 each.
The use of detection tubes is a method that can be employed by a small company or school district for a reasonable cost to obtain a fast determination as to whether a problem exists or not. However, a given tube will only detect a specific compound, so the problem material must be identified before the tube is chosen. This limits the value of the tubes as a diagnostic tool.
Getting a Read on Radon
The Environmental Protection Agency estimates that 10,000 to 20,000 persons per year die as a result of cancer caused, at least in part, by exposure to radon gas. Radon is an odorless, colorless, radioactive gas that occurs naturally in the earth. It is an element in the decay chain that starts with Uranium 238 and ends with stable lead. As a gas, radon migrates into basements and ground floor areas directly from the ground below. The concentration of radon in the air is measured in picoCuries per liter (piC/l). Levels of 4 to 20 piC/l warrant further investigation. If the measurement is over 100 piC/l, the EPA suggests that relocating the occupants (especially children) may be warranted.One of the most common methods of measuring radon is the "alpha-track" detector. This consists of a small strip of special plastic enclosed in a plastic container. Alpha radiation from the decay of radon gas and its byproducts leaves marks on the special plastic. These marks, or "tracks" are then counted under a microscope, and the average radon concentration is calculated from the number of these marks and the time the device was exposed.
Alpha track detectors cost under $100 and are good for long-term tests of up to 12 months. They are not suited for fast tests as they take at least a month to provide a reliable indication of radon presence.
Also available are charcoal canisters that are inexpensive and provide a faster indication than the alpha-track detectors. These devices contain activated charcoal that absorbs the radon gas over a period of two to seven days and is analyzed in a lab for radon content. The cost is similar to the alpha-track detectors. Charcoal canisters are faster than the alpha-track detectors but must have a stable indoor environment that might be hard to provide in heavily used public spaces.
The most expensive and fastest method of testing for radon is to hire a professional using a continuous measurement device. These devices use electronic components that sense the radiation emitted by radon gas. This information is converted into an indication of concentration. Attaching dataloggers allows the creation of a record of radon levels. These devices cost $5,000 or more and require skilled operation.
The Final Analysis
Tracking down the cause of IAQ problems can be a time-consuming task. But the use of skilled professionals helps the building operator do the job better and faster. If building occupants are complaining, use common sense methods first. These include complete inspections of the building for the storage of noxious chemicals, with an eye out for damp areas that might harbor microorganisms.After that, check hvac outdoor air intakes, condensation collectors, refrigerated beverage machines, and other possible sources of moisture.
If professionals are called, consult the EPA and local public agencies for guidance in the accreditation and licensure required for environmental testing. Quality service and a common sense approach will yield the best results for the building and its occupants.
