Many hospital systems and medical centers are experiencing an increased need for space to treat patients with behavioral health issues. According to the National Council for Behavioral Health, the demand for mental health and addiction services has increased significantly over the past year in part due to the impact of the COVID-19 pandemic. The Centers for Disease Control (CDC) has also weighed in with 2020 data that underscores the rise in mental health crises as a result of the pandemic, particularly for young people in the 18-24 age group.
As hospitals address this need for space, they must also consider the need for isolation rooms suited for behavioral health patients. Many patients are being admitted who require care for mental health issues while they are also COVID-19 positive. The need to treat and isolate COVID-19 patients displaying behavioral disorders is now an urgent facility need for hospitals throughout the U.S. At the same time, hospitals are faced with the dual challenge of addressing this need rapidly and cost-effectively, often with limited space options in existing suites.
Meeting Isolation Room Standards
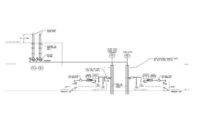
In an existing facility, HVAC retrofits to meet airborne infection isolation room requirements for infection control can be challenging. Negative air pressure helps prevent the droplet nuclei of airborne diseases, such as COVID-19, from escaping the room and infecting others. Airborne infection isolation rooms are designed to contain viruses within the room with air pulled into the room from corridors and then either exhausted directly to the outside or passed through a high-efficiency air (HEPA) filter before it is returned to circulation.
Vanderweil was recently tasked with retrofitting existing patient rooms in a behavioral health suite for a hospital in the Mid-Atlantic region. The rooms were used for isolation for patients with behavior health disorders but had not yet been properly converted to airborne infection isolation rooms. They were ventilated and conditioned via in-room induction units. Typical isolation rooms are designed for 100% exhaust, which, in most cases, requires the installation of new HVAC equipment and the need for additional shaft space on multiple floors to support the vertical distribution of new ductwork.
These new systems are expensive to retrofit and lead to increased energy consumption. As the rooms in question were to continue to be used for behavioral health patients, it was also important to address the need for any exposed equipment to minimize risk to patients.
After assessing a range of alternatives, and studying the constraints of the existing systems, capabilities, and space layouts, the Vanderweil team proposed a solution that included the installation of HEPA-filtered air purification systems and ultraviolet air modules that allow for the recirculation of air within the individual isolation unit. The exhaust system was upgraded to include new redundant fans on the roof with constant volume exhaust boxes dedicated for each isolation unit. This approach reduced the need for additional HVAC infrastructure and minimized disruption to the existing floor layouts.
As an added measure of safety, Vanderweil worked with the manufacturer of the supplemental units, Abatement Technologies, to address the potential need to modify the ceiling-mounted units for behavioral health settings. Abatement Technologies created a field-installed replacement kit for the door assembly that was shipped to the site.
Addressing Evolving Standards and Codes
This solution allows the hospital to use these rooms as isolation rooms for both COVID-19 patients and behavioral health patients, including those with both needs.
“Retrofits for the conversion of patient rooms to airborne infection isolation rooms require a close analysis of a confluence of codes, guidelines, and standards,” said Don Procz, P.E., LEED AP, principal at Vanderweil.
The Centers for Disease Control has updated its codes on isolation rooms in hospitals, and ASHRAE, the Facilities Guidelines Institute (FGI), American Institute of Architects (AIA), American Society of Health Care Engineering (ASHE) and other organizations all have standards to address.
“Health care facilities have always been highly regulated but the dual challenges of converting spaces to airborne infection isolation rooms and making them suitable for behavioral health patients require an extremely thoughtful approach,” said Procz. “The presentation of case studies and other avenues for evidence-based design and shared knowledge are extremely important as we navigate the current and evolving demands for safe and responsive health care settings that are part of the continuum of care.”