For nearly a century, scientists have known ultraviolet germicidal irradiation (UVGI or UV-C) energy deactivates airborne and surface-bound viruses, mycoplasma, bacteria, and fungi. Light in the 253.7-nm germicidal UV-C wavelength alters the protein structure in pathogens — DNA in bacteria and fungi, RNA in viruses — rendering the cell inactive and unable to replicate.
Through a process known as photodimerization, this genetic damage destroys a cell’s nucleic acids and protein structure by creating dimer lesions that prevent microorganisms from infecting and reproducing (see Figure 1). What’s more, this pathogen-deactivation process takes place without the creation of chemicals, volatile organic compounds (VOCs), or dangerous byproducts, such as ozone.
UV-C Marketplace
Prior to COVID-19, the UV-C market in the U.S. had seen continued growth, largely based on UV-C’s ability to maintain or restore HVAC system cooling coil capacity, which, in turn, increases airflow, lowers HVAC energy use, and reduces maintenance costs. The health care industry was an early adopter of UV-C technology, specifically wall-mounted upper-room fixtures that generate a germicidal zone near a room’s ceiling where infectious pathogens are quickly neutralized.
In the 1990s, facility managers began looking to UV-C fixtures to maintain HVAC heat transfer efficiency by inhibiting the proliferation of mold and gram-negative bacteria on, and through, the coil’s fins. This microbial buildup (known as biofilm) restricts airflow and the transfer of heat, forcing the entire HVAC system to work harder to compensate.This all changed once the pandemic struck. The ASHRAE Position Document on Infectious Aerosols identifies germicidal UV-C among a handful of scientifically proven technologies that can control airborne pathogens like the SARS-CoV-2 virus. Suddenly, the ability of UV-C to inactivate germs and viruses took on new significance, transforming the UV-C marketplace from an HVAC accessory to a health and safety necessity. See Figure 2 for an overview of the primary means of applying UV-C for air and HVAC surface protection against infectious agents.
Like other infectious diseases, such as tuberculosis, measles, SARS, and MERS, this new coronavirus is transmitted via airborne pathways. In April 2021, the U.S. Centers for Disease Control and Prevention (CDC) confirmed what some researchers had believed for months — the coronavirus is primarily communicated through airborne and not surface transmission.
The ASHRAE Epidemic Task Force (ETF) issued concurring counsel, acknowledging the risk of airborne transmission in its April 5, 2021, statement : “Airborne transmission of SARS-CoV-2 is significant and should be controlled. Changes to building operations, including the operation of HVAC systems, can reduce airborne exposures.”
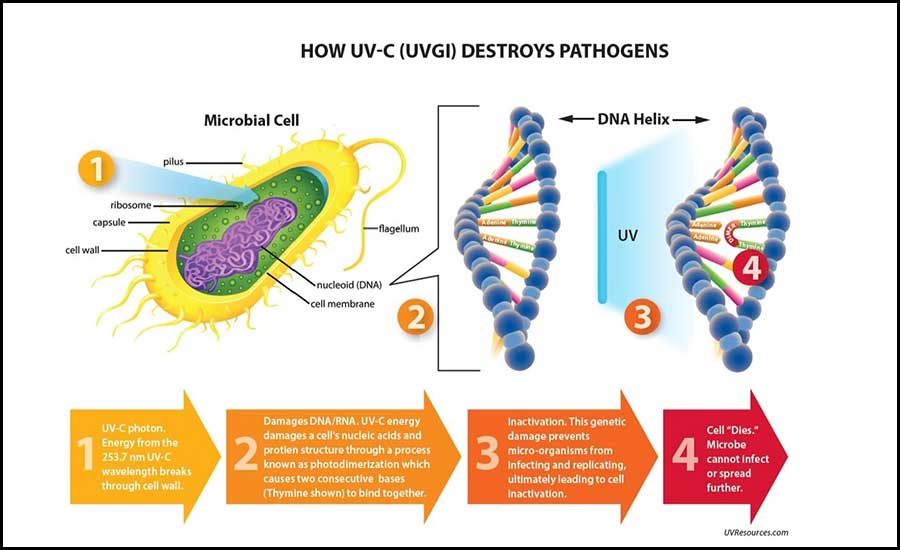 FIGURE 1: Through a process known as photodimerization, UV-C energy damages a cell’s nucleic acids and protein structure, causing two consecutive bases (Thymine shown) to bind together. This genetic damage prevents microorganisms from infecting and replicating, ultimately leading to cell inactivation. Images courtesy of UV Resources
FIGURE 1: Through a process known as photodimerization, UV-C energy damages a cell’s nucleic acids and protein structure, causing two consecutive bases (Thymine shown) to bind together. This genetic damage prevents microorganisms from infecting and replicating, ultimately leading to cell inactivation. Images courtesy of UV ResourcesVirus Transmission
It is this very issue — airborne pathogen spread — where germicidal UV became celebrated after researchers proved infection via the airborne route was possible and demonstrated the ability of UVGI to efficiently inactivate airborne microorganisms. In 1937, epidemiologist William F. Wells installed upper-room UV-C lamps (Figure 3) in suburban Philadelphia day schools to combat the spread of measles and compared infection rates to schools without UV-C. Schools equipped with the air-sanitizing equipment experienced a 13.3% infection rate compared with 53.6% for the population at large.
A 2020 study published in the American Journal of Infection Control found that, as for measles, influenza, and many other viruses, the 253.7-nm wavelength is effective in deactivating the SARS-CoV-2 virus:
- SARS-CoV-2 is highly susceptible to irradiation with ultraviolet light;
- High viral loads of 5-by-106 TCID50/ml SARS-CoV-2 can be inactivated in nine minutes by UV-C irradiation; and
- UVC irradiation represents a suitable disinfection method for SARS-CoV-2.
Importantly, researchers noted that successful deactivation of the SARS-CoV-2 virus by UV-C is not limited to laboratory settings, and virus inactivation extends to actual patient samples.
“We demonstrated that UV irradiation is a highly effective method to inactivate the new coronavirus SARS-CoV-2, even at the higher viral load levels that are found in research laboratories, e.g., in cell-culture supernatants or in diagnostic material taken from the respiratory tract of COVID 19 patients.”
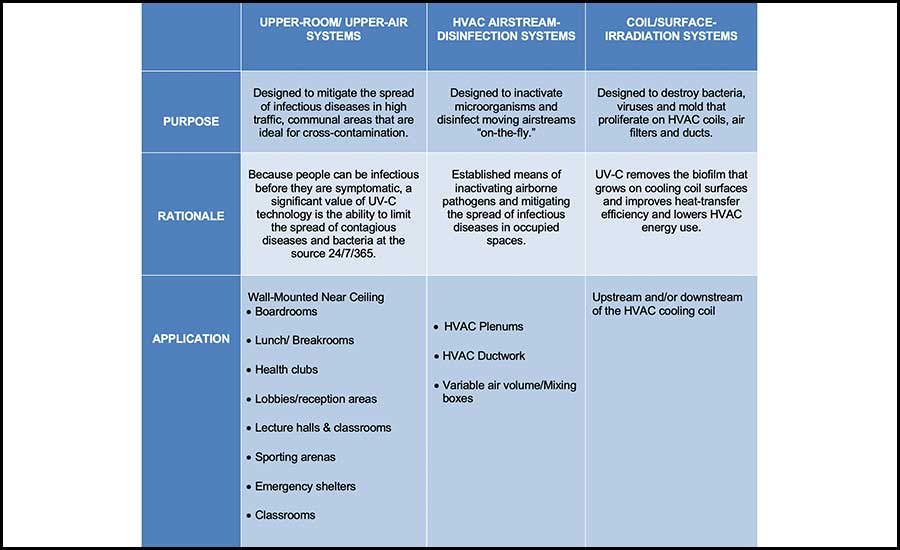 FIGURE 2: The selection of an air or surface disinfection system is based entirely on the application. Images courtesy of UV Resources
FIGURE 2: The selection of an air or surface disinfection system is based entirely on the application. Images courtesy of UV Resources
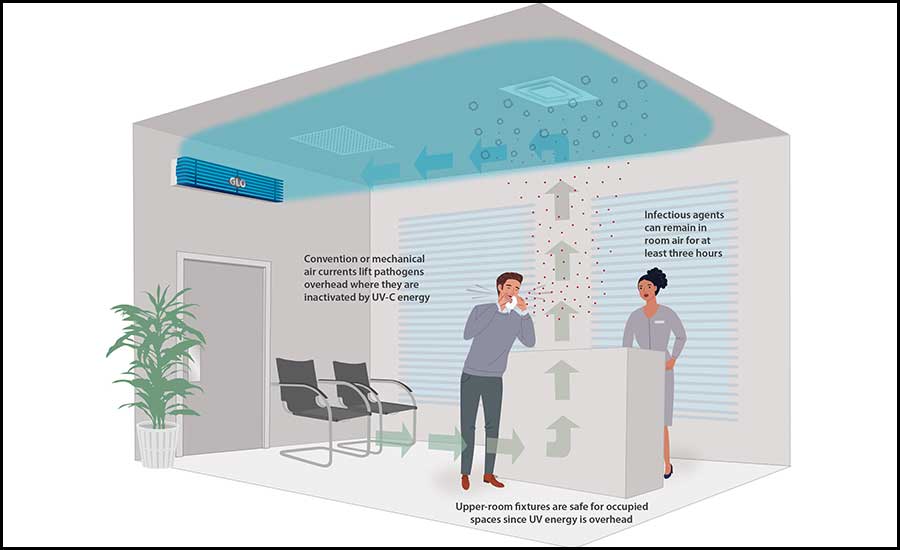 FIGURE 3: Upper-Room germicidal fixtures are wall-mounted 7 feet or above and use baffles to direct the UV-C energy upward and outward, ensuring that no UV-C energy enters the occupied portion of the room. Images courtesy of UV Resources
FIGURE 3: Upper-Room germicidal fixtures are wall-mounted 7 feet or above and use baffles to direct the UV-C energy upward and outward, ensuring that no UV-C energy enters the occupied portion of the room. Images courtesy of UV Resources
UV-C Residence Time
Bridging these findings from laboratory testing to real-world patient samples is significant, but what airborne virus stays put for nine minutes? Typical commercial HVAC air velocities are between 450-1,500 fpm, so HVAC UV-C disinfection systems have mere fractions of a second to deactivate pathogens (see Figure 4).
Luckily, there are multiple factors that influence microbial deactivation. The aforementioned photodimerization process relies upon a ratio of time and intensity, (e.g., how much residence time a pathogen is exposed to the UV-C energy will determine how much UV-C intensity is required.)
Here, we should clarify that different UV-C applications require different levels of germicidal exposure. For example, a stationary cooling coil receives UV-C energy 24/7/365, which is a high rate of exposure or residence time, so, therefore, the UV-C intensity can be lower. In the case of a moving airstream, however, exposure time is limited in some cases to fractions of a second, so UV-C intensity must be substantially greater.
Because microbial inactivation is a function of time and UV-C intensity, there are several site-specific factors that contribute to an airstream disinfection equation, including:
- Target pathogen and its susceptibility to UV-C (see Figure 5). The UV-C dose/fluence required to inactivate specific RNA and DNA viruses have been identified in various scholarly research dating back multiple decades to the present. These studies provide the necessary information/pathogen susceptibility that is used with predictive modeling to estimate how much UV-C is necessary to kill individual bacteria, viruses, or spores.
- The velocity of air traveling through the HVAC system, which will impact the length of exposure (residence time). A higher velocity of air requires greater intensity (more UV-C lamps) and/or a longer duct run to increase residence time. Said differently, as velocity increases beyond the typical 500 fpm, UV intensity must likewise increase. Conversely, less UV intensity would be required for air velocities below 500 fpm.
- The length of the plenum/duct — the longer the plenum or duct run, the better, as residence time and, thus, dose is increased.
- Air temperature — cold air can reduce the output of mercury vapor, and UV-C lamps and high relative humidity (RH) affect a pathogen's susceptibility to UV-C. Thus, airstream-disinfection measures can be more effective on the upstream side of a coil. In fact, moving UV-C lamps from 55°F temperatures (typical of downstream) to 75°F (typical of upstream) can increase a UV-C lamp’s output by as much as 40% or more. Although on-the-fly disinfection can be accomplished downstream of coils (see Figure 6), it typically requires greater UV-C fluence/intensity (e.g., more lamps).
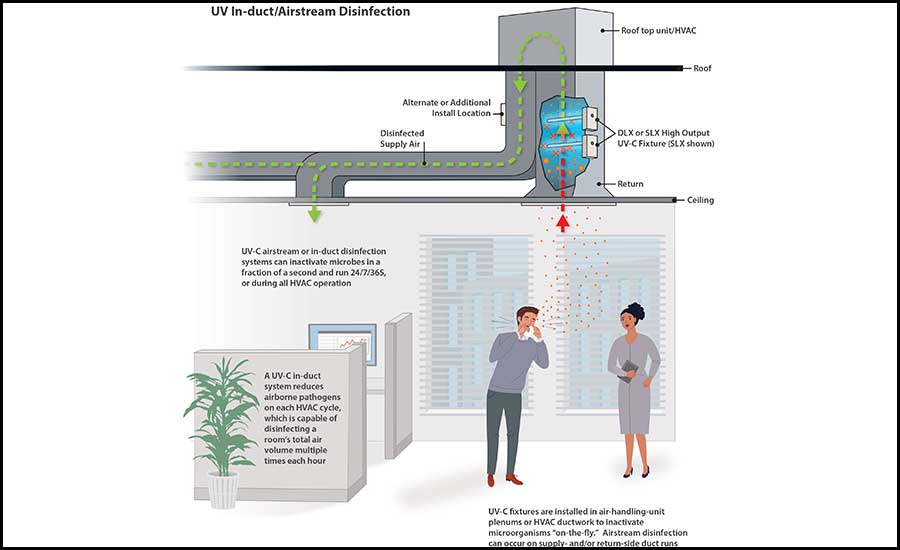 FIGURE 4: In-duct germicidal UV-C systems are installed in air-handling units or air distribution systems to inactivate microorganisms and disinfect moving airstreams “on-the-fly” as well as on HVAC surfaces. Images courtesy of UV Resources
FIGURE 4: In-duct germicidal UV-C systems are installed in air-handling units or air distribution systems to inactivate microorganisms and disinfect moving airstreams “on-the-fly” as well as on HVAC surfaces. Images courtesy of UV Resources
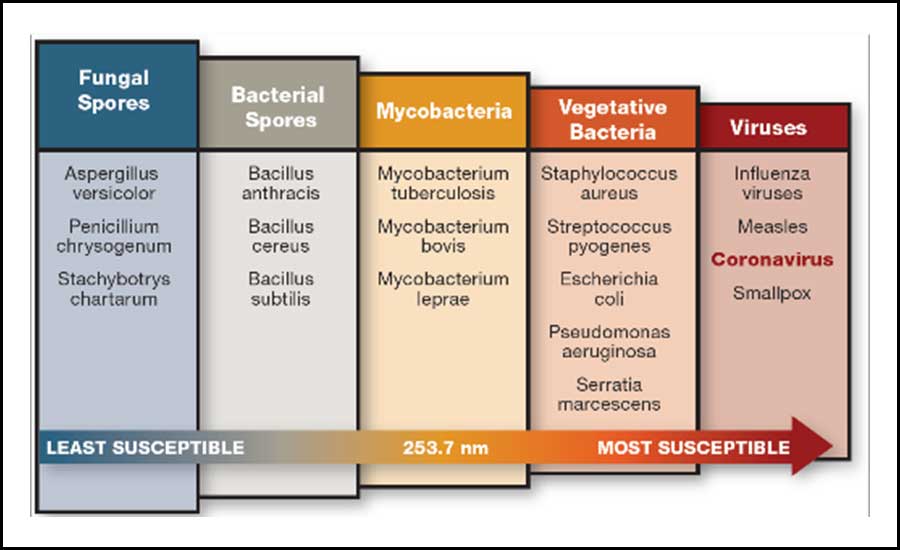 FIGURE 5: Germicidal UV-C inactivation of microorganisms by group. Data source: ASHRAE Handbook - HVAC Applications, Chapter 62. Images courtesy of UV Resources
FIGURE 5: Germicidal UV-C inactivation of microorganisms by group. Data source: ASHRAE Handbook - HVAC Applications, Chapter 62. Images courtesy of UV ResourcesSeparately, UV-C lamps are often encapsulated with a fluorinated ethylene propylene (FEP) coating or clear outer sleeve, which assists by insulating the lamp surface from air temperature changes. This protection can serve to increase lamp output and performance in extreme operating conditions of low temperatures and in high-velocity airstreams. It is estimated that between 50%-70% of building engineers order lamps with a similar UV-C transmissible “shatterproof” film or encapsulation, which also protects the AHU and airstream from glass and mercury residues should an accidental lamp break occur.
- Lamps — using more or higher output lamps will increase the total dose. UV-C systems with 360-degree irradiation allow more UV-C energy to saturate a plenum, increasing UV-C fluence.
- Reflectivity of the plenum — different metals boost the UV-C dose, as the germicidal wavelength “bounces” throughout the plenum and remains “in play” instead of being absorbed by surfaces. For example, most cooling coil fins are made from aluminum, which also assists with UV-C’s penetration into the coil to attack organic material within the coil. (see Figure 7).
- Fixture spacing — decreasing lamp-row spacing (e.g., from the surface-irradiation standard 36-inch centerlines to 15- to 18-inch centerlines) increases UV-C fluence.
Each of these factors will determine the amount of UV-C energy necessary in any given application (installations are typically modeled to help predict individual dosage levels). See Figure 8 for an example of how to calculate UVGI for air disinfection.
 FIGURE 6: When designing a germicidal UV disinfection system, engineers should consider the impact AHU location has on performance. Images courtesy of UV Resources
FIGURE 6: When designing a germicidal UV disinfection system, engineers should consider the impact AHU location has on performance. Images courtesy of UV ResourcesASHRAE and In-Duct Disinfection
For in-duct applications with limited exposure time, the ASHRAE ETF recommends the following guidelines for UV-C to deactivate the SARS-CoV-2 virus:
- Minimum target UV dose of 1,500 µW-s/cm2 (1,500 µJ/cm2);
- Systems typically designed for 500 fpm or slower moving airstream;
- Banks of UV lamps installed inside HVAC systems or ductwork positioned parallel or perpendicular to airflow;
- Minimum irradiance zone of 2 feet (24 inches);
- Minimum UV exposure time of 0.25 second; and
- Systems should be coupled with the highest practical MERV filter strength that does not compromise system performance.
The ASHRAE ETF has established a UV-C dose value of 1,500 µJ/cm2 to attain a 99% air inactivation rate for the SARS-CoV-2 virus. In practice, however, different environmental conditions, such as airflow speeds, air temperature and humidity levels, lamp aging, and system configuration, influence the strength of the antimicrobial dose. For example, as mentioned above, air temperature (cold air reduces the output of UV-C lamps); humidity (high RH decreases pathogen susceptibility to UV-C); and duct reflectivity all play a role in determining the amount of UV-C energy necessary in any given application. That’s why most installations are modeled by UV-C fixture manufacturers to help predict individual dosage levels.
Once these environmental factors are added to the predictive modeling, and based on prior peer reviewed studies, a target UV-C (254 nm) dose of 1,222 µJ/cm2 is estimated to achieve a 99% inactivation of the SARS-CoV-2 virus in air applications. Similarly, an estimated 90% inactivation rate would require a UV-C dose of 611 µJ/cm2.
Again, when designing an “on-the-fly” inactivation application, modeling the application’s site-specific conditions to ensure adequate UV-C dosage is recommended.
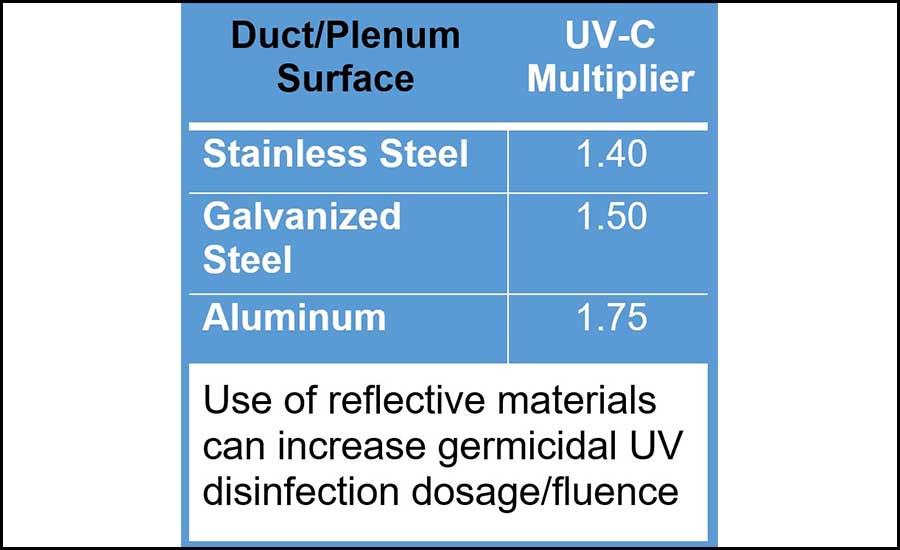 FIGURE 7: UV-C energy’s effectiveness is multiplied as it bounces off of the top, bottom, and sides of a plenum surface or coil fins. Images courtesy of UV Resources
FIGURE 7: UV-C energy’s effectiveness is multiplied as it bounces off of the top, bottom, and sides of a plenum surface or coil fins. Images courtesy of UV ResourcesConclusion
The COVID-19 pandemic has left no doubt that the 254-nm germicidal wavelength can inactivate the genetic material in the SARS-CoV-2 virus. Hundreds of scientific studies over the past century have proven the disinfectant efficacy of UV-C energy, having first inactivated viruses and other microbes on surfaces in 1877, in water in 1910, and in air in 1935.
In general, the effectiveness of UV-C air disinfection is a factor of time and intensity, and computer modeling helps ensure the necessary germicidal dose is achieved through a combination of UV-C energy exposure time and/or UV-C intensity.
To account for different environmental conditions, the ASHRAE ETF has set its conservative minimum UV-C dose value at 1,500 µJ/cm2 to attain a 99% air inactivation rate for the SARS-CoV-2 virus. As noted above, there are several operational factors that can increase the UV-C dosage or the cumulative amount of UV-C energy the pathogen receives. It is important to note that UV-C operates by line of sight; it can only inactivate what it can see (i.e., the inside of a closed drawer cannot be disinfected unless the contents of the drawer are exposed to the UV energy).
Infection preventionists recommend facility engineers and building managers use multilayer preventive infection-control measures, such as germicidal UV-C, to mitigate the potential spread of airborne diseases. A multi-barrier approach helps ensure that whatever pathogen is not mitigated by one method (say filtering) is inactivated by another (UV-C).
Recent guidance from ASHRAE, the CDC, and published technical articles in HVAC trade publications provide building engineers and facility staff with the resources needed to size, select, install, operate, and maintain UV airstream disinfection systems.
Author's note: All references to “disinfection” are referring generally to the UV-C germicidal inactivation of pathogenic biomass through the process of photodimerization and are not intended to refer to any specific definition by the U.S. Food and Drug Administration or EPA. In general, the effectiveness of UV-C air disinfection is a function of time and intensity, (e.g., how much time/duration a pathogen is exposed to the UV-C energy) as well as the amount of airflow (volume and velocity), the air temperature and RH, and the duct material reflectivity.
 FIGURE 8: Calculating UV-C airstream disinfection rates. Data Source: Kowalski, Wladyslaw. (2009). Ultraviolet Germicidal Irradiation Handbook. Images courtesy of UV Resources
FIGURE 8: Calculating UV-C airstream disinfection rates. Data Source: Kowalski, Wladyslaw. (2009). Ultraviolet Germicidal Irradiation Handbook. Images courtesy of UV Resources




